Peter Miller, M.D., Director of specialty Services at the hospital, was addressing James Gump, M.D., Chief Nephrologist
Question:
Peter Miller, M.D., Director of specialty Services at the hospital, was addressing James Gump,
M.D., Chief Nephrologist of Yarra’s Renal Division, concerning a change in Medicare’s payment
policies for hemodialysis treatments. Recently, Medicare had begun paying independent dialysis
clinics for standard dialysis treatments, and the change in policy had caused patient volume in
Yarra’s dialysis unit to decrease to about 50 percent of capacity, producing a corresponding
increase in per-treatment costs. By February of the current fiscal year, Dr. Miller and Yarra’s
Medical Director were considering closing the hospital’s dialysis unit.
A hospital just can’t afford to operate a department at 50 percent capacity. If we average 20
dialysis patients, it costs us $425 per treatment, and we’re only paid $250. If a department can’t
cover its costs, including a fair share of overhead, it isn’t self-sufficient and I don’t think we should
carry it.
Dr. Gump, who had been Chief Nephrologist since he’d helped establish the unit, was opposed to
closing it. Although he was impressed by the quality of care that independent centers offered, he
was convinced that Yarra’s unit was necessary for providing back-up and emergency services for
the outpatient centers, as well as for treatment for some of the hospital’s seriously ill inpatients.
Furthermore, although the unit could not achieve the low costs of the independent centers, he
disagreed with Dr. Miller’s cost figure of $425 per treatment. He resolved to prepare his own cost
analysis for their next meeting.
Background
Approximately 20 years ago, at Dr. Gump’s initiative, Yarra had opened the dialysis unit, largely
in response to the growing number of patients with chronic kidney disease. The hospital’s renal
division had long provided acute renal failure care and kidney transplants, but the most common
treatment for end-stage renal disease was hemodialysis. During dialysis, a portion of a patient’s
blood circulates through an artificial kidney machine and is cleansed of waste products. Used three
times a week for 4 to 5 hours, the kidney machine allows people with chronic kidney disease to
lead almost normal lives.
The dialysis unit had 14 artificial kidney machines. Because of space limitations, they used only
10 at any one time, reserving the other four for breakdowns and emergencies. Open 6 days a week
with two shifts of patients daily, the unit could provide 120 treatments a week, which mean they
could accommodate 40 regular patients.
From 1973, the year that Medicare began reimbursing for dialysis, all dialysis patients at Yarra
had been covered by Medicare. Until recently, the unit had operated at almost 100 percent capacity,
even extending its hours to accept emergency cases and to avoid turning away patients.
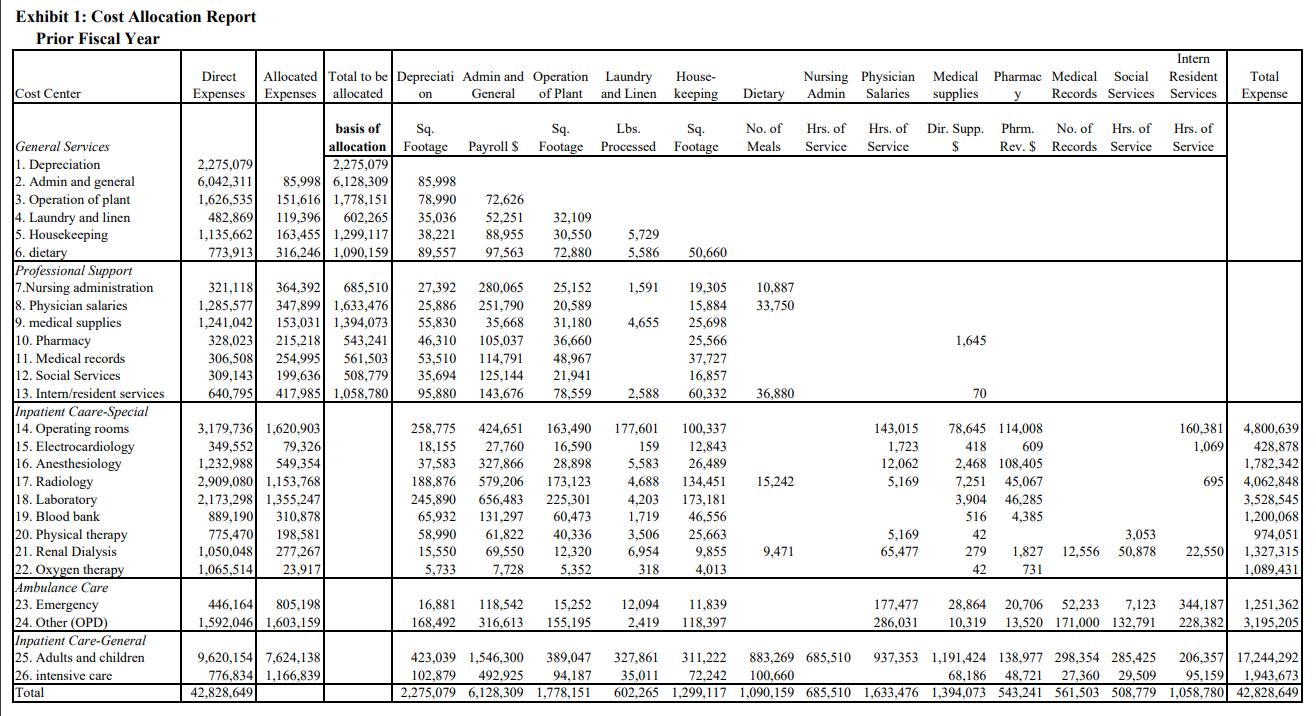
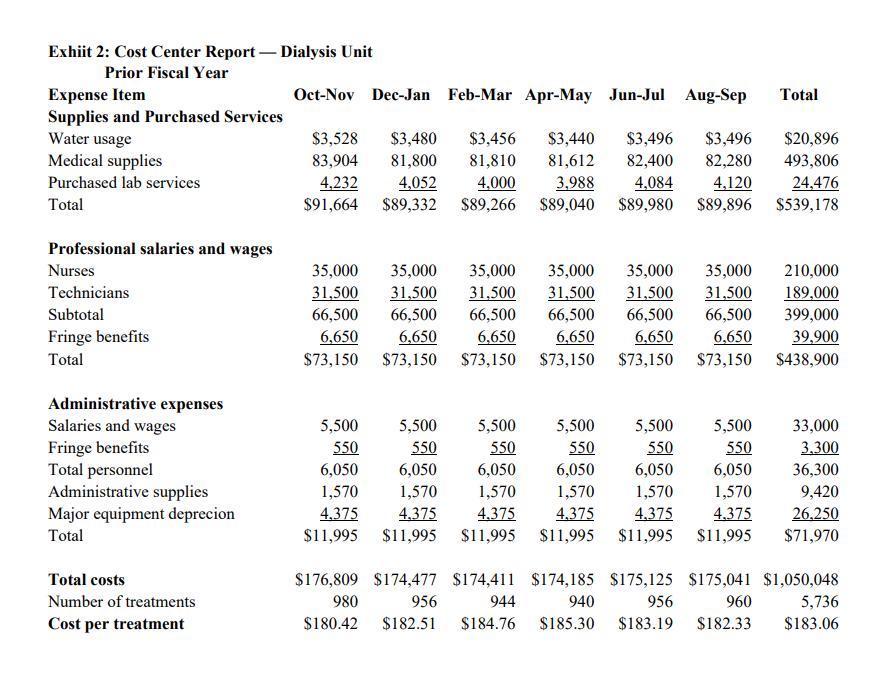
Patients typically spent their first three months of dialysis in a hospital facility. If there were no complications when this “start-up” period had passed, they were then required to transfer to an independent center. Most independent dialysis centers were centrally owned and operated, and were organized into satellite groups spread throughout urban and suburban areas. The facilities were modern and attractively designed and, because they were separate from hospitals’ institutional environments, they offered psychological advantages to patients. Centrally managed with low overhead, they could achieve economies unobtainable by similar hospital units. Supplies and equipment were purchased in bulk, for example, and administrators watched staff scheduling and other costs closely. As a result, their per treatment cots were significantly lower than those in a hospital facility. For example, a treatment in a center operating at 100 percent capacity with 40 patients could cost as little as $160. Yarra’s Data Yarra’s direct and allocated costs for the Renal Dialysis Unit in the previous fiscal year are detailed in Exhibit 1. Dr. Gump also obtained the unit’s cost center report for the same fiscal year (Exhibit 2), which provided a breakdown of the unit’s direct costs. Dr. Gump intended to use the prior year’s costs to calculate the pre-treatment cost at various volume levels for the current year. He also wanted to find the point at which the unit’s revenue would meet its costs. He commented: I plan to use only those costs that can be traced directly to dialysis treatments, and not any overhead costs. If the unit’s revenue meets its direct costs, it is self-sufficient. Peter’s treatment cost of $425 is misleading since it includes substantial overhead, and this year’s overhead will differ from last year’s because of the unit’s decrease in volume. Also, even though this year’s overhead can’t be calculated until the end of the fiscal year. I think I can come up with an estimate. First, though, I plan to calculate the “real” cost of a treatment and, from there, define a “fair share” of overhead. In reviewing the cost center report, Dr. Gump realized that the nature of the costs varied. There are three types of costs I need to consider in this analysis: those that vary in proportion to volume, those that vary with significant change in volume, and those that remain the same regardless of the unit’s volume. The first and the last are pretty clear. Medical supplies, purchased laboratory services, and water usage all change according to the number of treatments provided. The other non-professional personnel expenses will stay essentially the same regardless of the number of treatments. Salary and wages, and employee expense costs are more complicated. Although they didn’t change during the last year, the unit’s number of treatments also remain fairly steady. However, the significant reduction in volume this year might cause a corresponding reduction in salary and employee expenses. Last year, we employed seven hemodialysis technicians, seven nurses, and one administrator (our nephrologists are all on the hospital’s physicians’ payroll). However, since I had anticipated that volume would fall, I didn’t replace the nurse and two technicians who left in
January of this year. So, as of February, our annualized salaries have decreased by $84,000 and our fringe benefits have decreased by $8,400 for a total of about $92,400. When the operation is only at 50% of capacity, the staff can be reduced to one-shift operation (i.e., 4 nurses, 4 technicians, and 1 administrator). Finally, just as a precaution, in case Peter asks, I had my secretary call a hospital equipment supply manufacturer to discuss the resale value of our 14 machines. They told her that machines used for four years or more could not be sold, even for scrap. We purchased all 14 machines five years ago for $210,000.
Assignment 1. On a full-cost basis, how “profitable” was the dialysis unit last year? Please structure your answer in the form of a contribution income statement. (20%) 2. Dr. Miller says that it costs $425 per dialysis procedure. How did he calculate that figure? What, if anything, is wrong with his calculation? (10%) 3. Assume that the volume this year will be 3,120 procedures (20 patients, 3 time per week, 52 weeks in a year). At that level of volume, how profitable will the dialysis unit be this year? Be sure you calculate the new direct costs, and that you estimate, as best you can, this year’s allocated (or indirect) costs. (30%) 4. What is the unit contribution margin of a dialysis procedure? How might Dr. Gump use this number in thinking about his options? For example, how might he use it to calculate the “breakeven volume” of the dialysis unit? (10%) 5. Assume that Dr. Gump does not want Dr. Miller to eliminate the dialysis unit, how should he present his analysis? Please write a report to support Dr. Gump’s position. How do you think Dr. Miller will respond to this presentation? (30%)
Data:

Accounting for Decision Making and Control
ISBN: 978-1259564550
9th edition
Authors: Jerold Zimmerman




